Late Onset Tay-Sachs
- Details
-
Last Updated: Wednesday, 13 April 2016 15:53
Symptoms

First signs - Early symptoms of Late Onset Tay-Sachs (LOTS) include clumsiness and muscle weakness in the legs. Once diagnosed, adults often reflect back to their childhood and realize they experienced symptoms much earlier such as not being athletic, speech difficulties and/or a stutter as a child or teenager.
Mental health symptoms may present first which can lead to an especially long road to diagnosis. About 40% of affected adults experience mental health symptoms such as bi-polar or psychotic episodes.
Gradual Loss of skills - Over time adults with Late Onset Tay-Sachs slowly decline. Adults frequently require more mobility assistance, i.e. cane to walker to wheelchair. Many experience speech and swallowing difficulties but few require a feeding tube.
Long Road to Diagnosis
Late Onset Tay-Sachs may be hard to diagnose. Some adults go five or more years before learning their true diagnosis. In some cases it may be misdiagnosed as Multiple Sclerosis or ALS.
Adults affected by the adult form of Tay-Sachs do not exhibit the tell-tale cherry-red spot, which can contribute to a challenging and long road to diagnosis. Unfortunately many healthcare providers are not aware of the rare adult forms of these diseases and dismiss the initial diagnosis due to the age of the patient.
Adults that display mental health symptoms before physical symptoms often experience the longest road to diagnosis.
Tay-Sachs disease is diagnosed through a blood test to check the level of Hexosaminidase A (HexA). A follow-up DNA test may be recommended. Any doctor can order the Tay-Sachs HexA blood test. Often, a diagnosis is confirmed by a neurologist and/or geneticist, and after the completion of a metabolic evaluation.
Many affected adults express mixed emotions when finally receiving their diagnosis. After years of not knowing the cause of their progressive symptoms, they may experience a certain amount of relief when an accurate diagnosis is determined. At the same time, Tay-Sachs is a difficult diagnosis to receive and there can be a sense of regret and frustration.
Living with Late Onset Tay-Sachs
There is no treatment or cure for Tay-Sachs disease but there are ways to manage.
Mobility, speech and mental health are the primary symptom management issues of Late Onset Tay-Sachs. These symptoms frequently lead to other challenges related to employment, housing and communication. Click here to learn more about living with the disease.
Late Onset Tay-Sachs is a challenging and debilitating disorder but doesn't always shorten life span like the childhood forms of Tay-Sachs.
Read the "Topic of the Week" featuring the stories of two patients with Late Onset Tay-Sachs here.
Explore More:
 Research - the latest in Late Onset research
Research - the latest in Late Onset research
 Support - symptom management, where and how to find help, and how to cope.
Support - symptom management, where and how to find help, and how to cope.
 Causes - the missing HexA enzyme
Causes - the missing HexA enzyme
 History of Tay-Sachs Disease - named for Warren Tay and Bernard Sachs
History of Tay-Sachs Disease - named for Warren Tay and Bernard Sachs
Tay-Sachs Causes
- Details
-
Last Updated: Wednesday, 19 October 2016 08:39
It's about a missing enzyme.
Tay-Sachs disease is caused by the absence or significantly reduced level of a vital enzyme called beta-hexosaminidase. It is the Hexosaminidase A (HEXA) gene in the DNA that provides instructions for making this enzyme. Without the correct amount of the HexA enzyme, a fatty substance or lipid called GM2 ganglioside accumulates abnormally in cells, especially in the nerve cells of the brain. This ongoing accumulation, also called "substrate", causes progressive damage to the cells.
Infantile Tay-Sachs is typically the absence of the HexA enzyme. This differs from the Juvenile and Late Onset forms of Tay-Sachs when the mutations allow the HexA enzyme to function a little bit. Just a small increase in HexA activity is enough to delay the onset and slow the progression of symptoms.
Inheritance
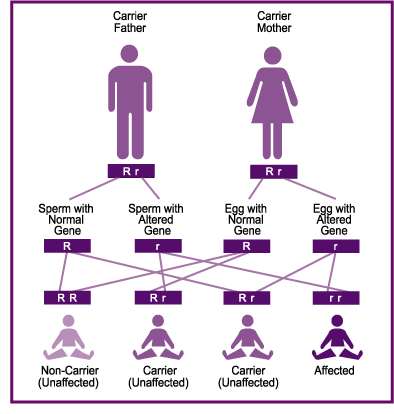
Tay-Sachs is an autosomal recessive genetic disorder. Autosomal means it affects males and females equally and recessive means both parents must be a carrier for the children to be at risk. If both parents are carriers, there is a 25% chance with each pregnancy that the child will be affected. Carriers of recessive diseases do not experience any adverse health effects. ANYONE can be a carrier of Tay-Sachs but French Canadians, Louisiana Cajuns and Ashkenazi Jews are at high risk with an carrier rate of 1/27. Some data suggests people of British Isle and Irish descent are at increased risk between 1/50 to 1/150. The Tay-Sachs gene occurs in the general population at a rate of 1/250.
Tay-Sachs "breeds true" in a family. If one child is diagnosed with Infantile Tay-Sachs, the other children are only at risk for the infantile form. One set of parents could not have children with both the infantile and juvenile forms of the disease.
Gene Location
The gene that causes Tay-Sachs is located on chromosome 15, specifically 15q23-q24.
 Read more About Inheritance
Read more About Inheritance
 Classic Infantile Tay-Sachs -Symptoms appear around 6 months of age.
Classic Infantile Tay-Sachs -Symptoms appear around 6 months of age. Juvenile Tay-Sachs -Symptoms typically appear between ages 2 and 5, but can occur anytime during childhood.
Juvenile Tay-Sachs -Symptoms typically appear between ages 2 and 5, but can occur anytime during childhood. Late Onset Tay-Sachs -Symptoms typically appear in adolescence or early adulthood, but can appear later.
Late Onset Tay-Sachs -Symptoms typically appear in adolescence or early adulthood, but can appear later. Causes - the missing HexA enzyme
Causes - the missing HexA enzyme Research - ongoing research
Research - ongoing research History of Tay-Sachs Disease - named for Warren Tay and Bernard Sachs
History of Tay-Sachs Disease - named for Warren Tay and Bernard Sachs


 Read more
Read more 